[et_pb_section admin_label=”Section” global_module=”2573″ fullwidth=”on” specialty=”off” transparent_background=”off” allow_player_pause=”off” inner_shadow=”off” parallax=”off” parallax_method=”off” make_fullwidth=”off” use_custom_width=”off” width_unit=”on” make_equal=”off” use_custom_gutter=”off”][et_pb_fullwidth_menu global_parent=”2573″ admin_label=”Type 1 Diabetes Menu” menu_id=”46″ background_color=”#ffecd2″ background_layout=”light” text_orientation=”center” submenu_direction=”downwards” fullwidth_menu=”off” dropdown_menu_animation=”fade”] [/et_pb_fullwidth_menu][/et_pb_section][et_pb_section admin_label=”Section” fullwidth=”off” specialty=”off”][et_pb_row admin_label=”Row”][et_pb_column type=”2_3″][et_pb_text admin_label=”Text” background_layout=”light” text_orientation=”left” use_border_color=”off” border_color=”#ffffff” border_style=”solid”]
Introduction
Type 1 diabetes (T1D), also known as Diabetes mellitus type 1 or juvenile diabetes, occurs when the body’s immune system attacks the insulin-producing beta cells in the pancreas and destroys them. The pancreas then produces little or no insulin.
Insulin is a hormone, a chemical messenger that is transported in the blood and regulates important body functions. Without insulin your body cannot get the energy it needs from the food you have eaten. This vital hormone is usually produced in the pancreas and released into the bloodstream. Here it enables the sugar (glucose) in our food and drink to be transported into our cells and converted into energy for our bodies.
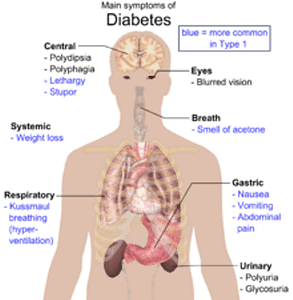 Without insulin our bodies cannot use the sugar in our blood, so the sugar builds up there. This is known as hyperglycemia. Very high blood sugar concentrations cause a number of symptoms, including frequent urination, feeling very thirsty, tiredness, listlessness, nausea and dizziness. If someone has extremely high blood sugar levels, they may feel confused and drowsy or even lose consciousness (diabetic coma). The long term effects of T1D can also include damage to the capillaries, which over time can lead to blindness or kidney failure. Nerves can also be damaged by long term disease, leading to the development of wounds which heal slowly due to poor blood supply.
Without insulin our bodies cannot use the sugar in our blood, so the sugar builds up there. This is known as hyperglycemia. Very high blood sugar concentrations cause a number of symptoms, including frequent urination, feeling very thirsty, tiredness, listlessness, nausea and dizziness. If someone has extremely high blood sugar levels, they may feel confused and drowsy or even lose consciousness (diabetic coma). The long term effects of T1D can also include damage to the capillaries, which over time can lead to blindness or kidney failure. Nerves can also be damaged by long term disease, leading to the development of wounds which heal slowly due to poor blood supply.
Because the pancreas produces little or no insulin in patients with T1D, patients must inject insulin every day to get the insulin they are lacking. Good management of T1D is important in order to avoid the symptoms of hyperglycemia.
To diagnose T1D, blood samples can be taken to measure the patient’s sugar level. To see whether someone’s blood sugar levels have been too high over a longer period of time, something known as the Hemoglobin A1c value is measured. This value indicates how high your blood sugar has been on average in the last two to three months. Sometimes ketone testing of the blood or urine is performed to diagnose T1D.
Cause of Type 1 Diabetes
T1D makes up about 5-10% of all diabetes cases. Between 11 and 22 million people are affected worldwide. T1D cases have been increasing at a rate of about 3% per year. The tendency to develop autoimmune diseases, including type 1 diabetes, can be passed down through families. T1D develops most often in young people but can appear in adults.
The ultimate cause of T1D is the destruction of the insulin-producing beta cells of the pancreas by the immune system. Over time the beta cells become so damaged that they produce very little insulin or none at all. What causes the immune system to attack the beta cells initially has been the subject of much research and debate. An infection or another trigger causes the body to mistakenly attack the cells in the pancreas that make insulin. A combination of genetic and environmental factors is likely as well.
More than 50 genes have been associated with T1D. The risk of developing type 1 diabetes is increased by certain variants of the HLA-DQA1, HLA-DQB1, and HLA-DRB1 genes. These genes provide instructions for making proteins that play a critical role in the immune system. They belong to a family of genes called the human leukocyte antigen (HLA) complex. The HLA complex helps the immune system distinguish the body’s own proteins from proteins made by foreign invaders such as viruses and bacteria. These genetic variants seem to increase the risk of an inappropriate immune response to beta cells. However, they are also found in the general population, and only about 5 percent of individuals with the gene variants develop T1D. HLA variations account for approximately 40 percent of the genetic risk for the condition. Other HLA variations appear to be protective against the disease. Changes in the HLA region have also been associated with multiple sclerosis, celiac disease and lupus.
Treatment of Type 1 Diabetes
 There is no way to prevent T1D. Monitoring and maintaining stable blood sugar levels with insulin treatments is critical for survival. Many patients treat T1D with daily insulin injections, but some use an insulin pump.
There is no way to prevent T1D. Monitoring and maintaining stable blood sugar levels with insulin treatments is critical for survival. Many patients treat T1D with daily insulin injections, but some use an insulin pump.
There are four types of insulin, categorized based on the speed and duration of action:
- rapid acting insulin
- short acting insulin
- intermediate acting insulin
- long acting insulin
Diet and exercise are also important considerations in treating T1D. A low carbohydrate diet has been shown to be beneficial in managing T1D. Managing stress levels improves T1D. Pancreas and islet cell transplantation are less common options for patients who are not well controlled by insulin therapy. The risks of these surgeries are considerable, and the success rate of islet cell transplantation was 44%.
[/et_pb_text][/et_pb_column][et_pb_column type=”1_3″][et_pb_button admin_label=”2017 MAP Conference” global_module=”3207″ saved_tabs=”all” button_url=”http://humanpara.org/2017-map-conference/” url_new_window=”on” button_text=”2017 MAP Conference” button_alignment=”center” background_layout=”light” custom_button=”on” button_text_color=”#081739″ button_bg_color=”#ffaa3c” button_letter_spacing=”0″ button_font=”Georgia|on|||” button_use_icon=”default” button_icon=”%%289%%” button_icon_color=”#081739″ button_icon_placement=”right” button_on_hover=”off” button_letter_spacing_hover=”0″] [/et_pb_button][et_pb_image admin_label=”Donate CCLLC” global_module=”3077″ saved_tabs=”all” src=”https://mlhn7gtupcl6.i.optimole.com/w:auto/h:auto/q:mauto/f:best/http://humanpara.org/wp-content/uploads/2017/01/HPF_Website_Image_DONATE.png” show_in_lightbox=”off” url=”/site-donate/” url_new_window=”off” use_overlay=”off” animation=”off” sticky=”off” align=”center” force_fullwidth=”on” always_center_on_mobile=”on” use_border_color=”off” border_color=”#ffffff” border_style=”solid”] [/et_pb_image][et_pb_image admin_label=”Facebook Button” global_module=”3072″ saved_tabs=”all” src=”https://mlhn7gtupcl6.i.optimole.com/w:auto/h:auto/q:mauto/f:best/http://humanpara.org/wp-content/uploads/2017/01/HPF_Website_Image_FACEBOOK.png” show_in_lightbox=”off” url=”https://www.facebook.com/The-Crohns-Infection-977765988963098/” url_new_window=”on” use_overlay=”off” animation=”off” sticky=”off” align=”center” force_fullwidth=”on” always_center_on_mobile=”on” use_border_color=”off” border_color=”#ffffff” border_style=”solid”] [/et_pb_image][et_pb_video admin_label=”Video” src=”https://www.youtube.com/watch?v=1Mf7KtDquyM&feature=youtu.be”] [/et_pb_video][et_pb_signup admin_label=”CCLLC Signup” global_module=”2535″ saved_tabs=”all” provider=”mailchimp” mailchimp_list=”9df80aedbc” aweber_list=”none” title=”Register for our Newsfeed” button_text=”Register” use_background_color=”on” background_color=”#e0ecff” background_layout=”light” text_orientation=”left” use_focus_border_color=”off” use_border_color=”off” border_color=”#ffffff” border_style=”solid” custom_button=”on” button_text_color=”#07163b” button_bg_color=”#ffab03″ button_border_color=”#07163b” button_border_radius=”8″ button_letter_spacing=”0″ button_use_icon=”default” button_icon=”%%32%%” button_icon_placement=”right” button_on_hover=”on” button_letter_spacing_hover=”0″]
Get Your News and Updates
Please enter your information and you will be added to the list
Your information will never be shared or sold!
[/et_pb_signup][/et_pb_column][/et_pb_row][/et_pb_section][et_pb_section admin_label=”Section” fullwidth=”on” specialty=”off” transparent_background=”off” allow_player_pause=”off” inner_shadow=”off” parallax=”off” parallax_method=”off” make_fullwidth=”off” use_custom_width=”off” width_unit=”on” make_equal=”off” use_custom_gutter=”off”][et_pb_fullwidth_slider admin_label=”Fullwidth Slider” global_parent=”2537″ show_arrows=”on” show_pagination=”off” auto=”off” auto_ignore_hover=”off” parallax=”off” parallax_method=”off” remove_inner_shadow=”off” background_position=”default” background_size=”default” hide_content_on_mobile=”off” hide_cta_on_mobile=”off” show_image_video_mobile=”off” custom_button=”on” button_letter_spacing=”0″ button_use_icon=”default” button_icon_placement=”right” button_on_hover=”on” button_letter_spacing_hover=”0″ top_padding=”10px” bottom_padding=”40px” button_text_size=”24″ button_text_color=”#081739″ button_bg_color=”#ffffff” button_font=”Georgia|on|||”] [et_pb_slide button_text=”MAP and T1D” button_link=”http://humanpara.org/map-and-type-1-diabetes/” background_position=”default” background_size=”default” background_color=”#ffaa3c” use_bg_overlay=”off” use_text_overlay=”off” alignment=”center” background_layout=”dark” allow_player_pause=”off” text_border_radius=”3″ header_font_select=”Georgia” header_font=”Georgia||||” body_font_select=”default” body_font=”||||” custom_button=”off” button_font_select=”default” button_font=”||||” button_use_icon=”default” button_icon_placement=”right” button_on_hover=”on”] [/et_pb_slide] [/et_pb_fullwidth_slider][/et_pb_section]
